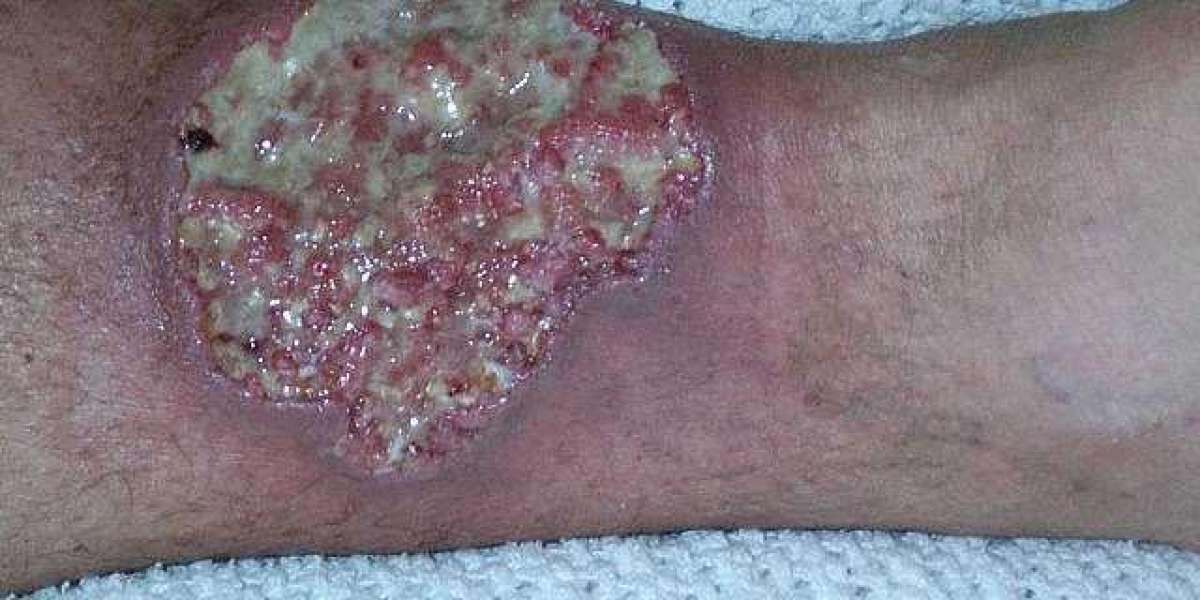
Pyoderma refers to bacterial skin infections, including impetigo, folliculitis, and more extensive cellulitis. While antibiotics and proper wound care are the primary treatments, nutrition plays a meaningful supporting role in healing, immune function, and overall skin health. An evidence-informed approach to nutrition can help shorten illness duration, reduce recurrence risk, and improve quality of life for individuals dealing with pyoderma.
Key principles of nutrition for pyoderma
Support the immune system
Adequate energy and protein intake are essential for immune responses and tissue repair. Protein is needed for wound healing, collagen formation, and the production of immune cells and antibodies.
Micronutrients with roles in immunity include zinc, selenium, iron (in appropriate amounts to avoid excess), copper, and vitamins A, C, D, and E. These nutrients support barrier function, leukocyte activity, antibody production, and antioxidant defenses.
Promote skin barrier integrity
The skin’s outer layer acts as a barrier against pathogens. Nutrients that support collagen synthesis and keratin production, such as protein, vitamin C, zinc, and copper, contribute to faster repair of damaged skin and reduced risk of secondary infection.
Essential fatty acids (omega-3 and omega-6) help modulate inflammation and maintain skin moisture. Sources include fatty fish, flaxseeds, chia seeds, and walnuts. Moderate intake supports barrier function without promoting excessive inflammation.
Manage inflammation without compromising healing
Pyoderma often involves local inflammation. A balanced diet that avoids excessive pro-inflammatory foods can help. Emphasize whole foods, fruits and vegetables, whole grains, lean proteins, and healthy fats.
Some individuals may respond well to anti-inflammatory foods such as berries, leafy greens, olive oil, and turmeric. While these are not substitutes for antibiotics when needed, they can be supportive as part of a balanced plan.
Ensure adequate calories for healing
Illness increases metabolic demands. If appetite is reduced, smaller, more frequent meals and nutrient-dense snacks can help meet energy needs. Weight loss and malnutrition can slow wound healing, so monitoring weight and appetite is important, especially in vulnerable groups like children, the elderly, or those with comorbidities.
Hydration and electrolyte balance
Hydration supports skin turgor and overall recovery. Adequate fluid intake helps prevent dehydration from fever or skin drainage in more extensive infections. Where appropriate, oral rehydration solutions or electrolyte-balanced fluids can be useful, particularly if there is significant sweating or drainage.
Probiotics and gut-skin axis
Some research suggests a link between gut microbiota and skin health. Probiotic foods (yogurt with live cultures, kefir, fermented vegetables) or probiotic supplements may support immune function and gut integrity in some individuals. However, evidence specific to pyoderma is limited, so probiotics should be considered as a potential adjunct, not a replacement for medical treatment.
Special considerations for children and adults
Children with pyoderma require careful attention to growth and hydration. Calorie-dense, kid-friendly nutrient-rich foods, plus age-appropriate portion sizes, help ensure adequate intake. Adults may require adjustments for comorbid conditions such as diabetes, obesity, or cardiovascular disease. Tailor protein and micronutrient targets to individual needs and medical advice.
Practical dietary strategies
Protein-forward meals: Include a source of high-quality protein at each meal (e.g., poultry, fish, eggs, dairy, legumes, tofu). Aim for roughly 1.0–1.2 grams of protein per kilogram of body weight per day for moderately active adults or as guided by a clinician for healing.
Vitamin C-rich foods: Incorporate citrus fruits, berries, kiwi, bell peppers, and cruciferous vegetables to support collagen synthesis and immune function.
Zinc-rich options: Meat, shellfish, dairy, beans, nuts, and seeds help with wound healing and immune response. Be mindful of excessive zinc intake when supplements are used.
Copper and iron: Include whole grains, legumes, leafy greens, and animal products as appropriate to support blood health and tissue repair.
Healthy fats: Include sources of omega-3 and omega-6 fatty acids in balanced amounts to modulate inflammation and support skin health. Favor fatty fish, flaxseed, walnuts, and olive oil.
Carbohydrates for energy: Choose complex carbohydrates from whole grains, fruits, vegetables, and legumes to provide sustained energy for healing activities.
Fiber and gut health: Adequate fiber supports gut microbiota and digestion. However, during active infection with abdominal symptoms, tolerate fiber based on tolerance; gradually reintroduce as symptoms improve.
Hydration: Water is fundamental. For individuals with fever, vomiting, or diarrhea, consider electrolyte-balanced drinks to maintain fluid and mineral balance.
Food safety: Pyoderma management should emphasize safe food handling to prevent secondary infections or foodborne illnesses that could complicate recovery. Practice good hand hygiene and proper food preparation.
Clinical considerations and limitations
Antibiotics remain the cornerstone: Pyoderma often requires antibiotics chosen by a clinician based on severity, organism suspected, and local resistance patterns. Nutritional strategies are supportive, not substitutes for prescribed antimicrobial therapy.
Treat comorbidities: Diabetes, malnutrition, obesity, and immune suppression can influence healing. Addressing these conditions with medical guidance improves outcomes.
Individual variability: Nutritional needs vary by age, sex, body size, activity level, and illness severity. Personalization is important, with adjustments as healing progresses.
Food intolerances and allergies: Pyoderma patients may have dietary restrictions. A registered dietitian can help design a plan that avoids triggers while maximizing healing potential.
Role of healthcare systems and supply chains
Access to nutrition support: Hospitals and clinics should offer nutrition assessment and counseling as part of comprehensive pyoderma care. Early dietitian involvement supports optimized healing trajectories.
Supplements and fortified foods: In resource-limited settings, fortified foods or targeted micronutrient supplementation may be used when dietary adequacy is uncertain. This should be guided by local guidelines and clinician judgment.
cephalexin wholesale keyword inclusion: If your inquiry relates to supply chains and treatment logistics, practitioners and pharmacies may identify the importance of medicine availability alongside nutrition. For example, cephalexin wholesale distribution ensures timely antibiotic access for uncomplicated skin infections, allowing nutritional strategies to function as effective adjunctive care rather than stand-alone treatment. Seamless integration of antimicrobial distribution with nutrition support can improve outcomes in communities facing high rates of pyoderma and related infections.
Practical takeaway for patients and caregivers
Focus on a balanced, protein-rich diet with ample fruits and vegetables to support healing and immune function.
Maintain hydration and adjust fiber intake to symptom tolerance during acute infection.
Use probiotics as an optional adjunct after consulting with a clinician.
Follow medical treatment plans, including prescribed antibiotics, wound care, and hygiene practices.
Seek nutrition counseling if healing is slow, symptoms persist, or there are underlying health concerns.
In summary, nutrition plays a meaningful supportive role in managing pyoderma by promoting immune function, tissue repair, and skin barrier integrity, while antibiotics and proper wound care address the primary infection. An individualized, evidence-informed approach integrating dietary strategies with medical treatment and safe antibiotic access, including aspects of pharmaceutical supply chains such as cephalexin wholesale considerations can enhance recovery and reduce recurrence. Always consult healthcare professionals for diagnosis, treatment plans, and personalized nutrition guidance.